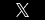When most people think of IKEA, they think of affordable, sleek, modern furniture that customers assemble themselves. However, three recent tragedies may change the way some of us think about the stylish Swedish furniture company. Three wrongful death cases have been filed against IKEA for the deaths of three toddlers who were crushed when defective dressers fell onto them. The lawsuits, for three separate incidents, were filed in the state court in Pennsylvania. IKEA has agreed to settle the lawsuits, which claim the company was negligent in its manufacturing of the dressers, for $50 million.
Although these recent tragedies are especially disturbing, they are not the only wrongful death lawsuits filed against IKEA for defective furniture. In fact, there have been a total of seven deaths linked to the company’s unstable furniture. Further, new evidence shows that IKEA may have known about the risk of death. If you have been injured by a defective product, contact a Boston injury lawyer today.
In the cases involving the three toddlers, IKEA initially denied blame, arguing that the parents were at fault for not properly anchoring the dressers to a wall. The manufacturer’s assembly instructions did, indeed, include this last step. However, the court ruled in favor of the victims’ families, saying that consumers commonly ignore instructions to anchor furniture to a wall. Although this last step may provide better stability, a reasonable person wouldn’t think that ignoring it would result in the death of a child. User error is certainly taken into account in defective product cases, however, it can only go so far. In the above cases, a warning to anchor the dresser was not sufficient to insulate the company from liability.
Massive IKEA Recall
Earlier this year, nearly 30 million IKEA dressers were recalled because they didn’t meet safety and stability standards. In addition to the recall and the large settlement, IKEA is increasing efforts to raise awareness about the importance of furniture anchoring through its “Secure It” program. If you’ve been injured by a defective product, contact a MA injury lawyer today.
The Four Elements of a Defective Product Liability Claim
If you have suffered personal injury or property damage because of a product, you may have a defective product liability claim. To win your case, you must prove that the elements below existed:
- You were injured or suffered a loss as a result of using the product
- The product was defective
- The product’s defect directly caused your injury
- You were using the product for its intended use
If any of these elements did not exist, you may have a difficult time winning a defective product lawsuit. With the help of a skilled defective product attorney, however, your chances of a successful lawsuit are dramatically improved. Defective product liability is a complex area of the law; find an attorney who has extensive experience in this specific area. Continue reading
 Boston Injury Lawyer Blog
Boston Injury Lawyer Blog